Stress Fractures
What is a stress fracture?
A stress fracture is a microscopic fracture of the bone that is so small that it often cannot be picked up on X-ray. If left untreated, a stress fracture can cause significant disability and develop into a full fracture, possibly even requiring surgery.
The majority of stress fractures occur in the lower limb, being particularly common in the hip, shins and foot at points where the most force passes through when weight bearing. Most stress fractures are overuse injuries and are common in long distance runners.
What are the symptoms?
As with many overuse injuries, the pain of a stress fracture starts gradually, beginning with pain during or after activity or sometimes the morning after. If activity continues without modification, the pain will gradually increase. Eventually most people are unable to maintain their usual activity level. Stress fractures are common in runners and military personnel who are required to march for long periods. A stress fracture will be more likely to occur in a person who has weaker bone strength, such as someone with osteoporosis, which is itself affected by many factors such as adequate calcium intake, vitamin D deficiency and a history of inactivity.
How are stress fractures treated and how long will it take to get better?
Stress fractures can easily be mistaken for other conditions such as shin splints. As the fracture is often too small to show up on X-ray, definitive diagnosis can be made using MRI or bone scan.
After diagnosis, the most important part of treatment will be resting the area to allow the bone to heal before resuming activity. Stress fractures usually need at least 6 weeks to recover fully. Some areas of the body have poor blood supply, which makes healing more complicated. For example, stress fractures of the navicular bone of the foot may need to be kept still and placed in a boot or cast for a period of time to heal properly.
Other aspects of treatment will involve correcting any factors that contributed to the original injury. There is some evidence that unsupportive footwear is a risk factor, along with poor biomechanics and weak muscles that provide inadequate support to the skeletal system during activity. Speak to your physiotherapist if you suspect you may have a stress fracture or simply want to know more.
None of the information in this article is a replacement for proper medical advice. Always see a medical professional for advice on your individual injury.



 What is it?
What is it? Our muscles play an important role in the movement of our body. Without our muscles, we wouldn’t be able to bend our elbow or straighten our leg. As our muscles are soft and designed for flexibility, they are also prone to injury and if you have ever had a muscle tear, you know that they can be surprisingly painful.
Our muscles play an important role in the movement of our body. Without our muscles, we wouldn’t be able to bend our elbow or straighten our leg. As our muscles are soft and designed for flexibility, they are also prone to injury and if you have ever had a muscle tear, you know that they can be surprisingly painful.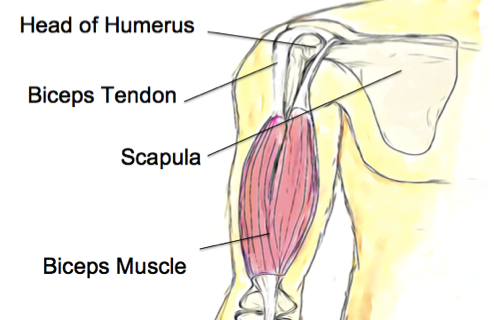 What is it?
What is it? Low back pain (LBP) is thought to affect up to 60 to 80% of the Western population throughout the course of their life. Many people do not have any preceding events to cause this back pain, although specific injuries can also initiate their symptoms. Lower back pain constitutes almost half of all chronic pain. This has a huge effect on quality of life and people with LBP tend to have more time off work and higher of medical costs than those who do not have symptoms.
Low back pain (LBP) is thought to affect up to 60 to 80% of the Western population throughout the course of their life. Many people do not have any preceding events to cause this back pain, although specific injuries can also initiate their symptoms. Lower back pain constitutes almost half of all chronic pain. This has a huge effect on quality of life and people with LBP tend to have more time off work and higher of medical costs than those who do not have symptoms. What is it?
What is it?
